
Concerns about a lack of medical training positions in the future
Reports such as Health Workforce Australia’s Doctors in Focus are not the first source of information reporting a maldistribution of doctors in Australia, with more doctors practising in major cities than regional and remote locations. With some universities such at Charles Sturt and Latrobe pushing for a new medical school in a regional location to be part of the solution to the shortage of rural doctors in New South Wales and Victoria, it seems simple. Follow in the footsteps of (regionally located medical school) James Cook University graduates, where many graduates go on to work in non-metropolitan areas. Let’s look at why simply training more medical students might not be the answer……
There is no doubt that there are more doctors in major cities than more regional and remote locations. Putting together the data from the Doctors in Focus and the Australian Institute of Health and Welfare’s Medical Workforce 2011 reports, in Australia, per 100,000 population, the number of full-time equivalent doctors was: 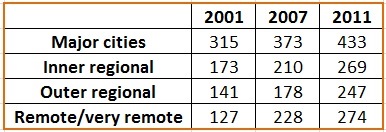
The James Cook University Medical School opened in Townsville in 2000. Student placements are based in Townsville, Cairns, Mackay and Darwin, with the opportunity for rural/remote placements in Australia as well as international placements. According to a recent report, more than two thirds of James Cook University medical graduates are working in non-metropolitan areas, six to seven years after qualifying as doctors. So with evidence suggesting that having medical schools in regional centres (where post-graduate training is also available in a nearby regional centre) wouldn’t it make sense to open more of these medical schools to produce graduates who become doctors in rural and remote areas?
Yes.
But……
The issue is in the sheer number of medical students coming through the system. The Australian Medical Association has called it a tsunami. In Australia in 2000, there were 1,195 medical graduates, and in 2013, the number expected is 3,556. That’s an increase of almost 300%. Where it gets “interesting” is in what happens after these medical students graduate. To become a fully qualified doctor, they must complete an internship, residency, and then become a registrar. That is, stay on the pathway until they have completed their advanced training to become a specialist such as a dermatologist, anaesthetist, ophthalmologist or general practitioner (GP).
Those of you who have followed the issues in medical training for a little while will remember the intern crisis of 2012. In 2012 there were over 100 international students who had completed their medical degrees in Australia who were set to miss out on internships for 2013. The Labor Federal Health Minister Tanya Plibersek announced a one-off last minute round of funding of $10 million to cover these internships.
Before the 2013 federal election, Peter Dutton announced that if elected, the Liberals would provide $40 million for an extra 400 medical internships for 2014. At the time of publishing this article, My Health Career had not heard of any 2013 medical graduates from Australian universities missing out on internships for 2014. Peter Dutton ensured that any international students were catered for with the Commonwealth Medical Internship program in October 2013.
What this tells us is that so far, both of the major Australian political parties have come to the rescue by providing internships for medical graduates when they were required. The medical training system does have a significant chance for volatility though, as essentially you have the Federal Government providing internships for a state-run hospital/health system.
The next hurdle for medical graduates may come in the form of registrar positions in the coming years. 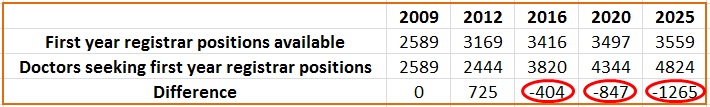
Health Workforce Australia’s report Health Workforce 2025: Doctors, Nurses and Midwives Volume 1 shows that if nothing changes in the medical training system, there will be a shortage of 404 (10.6%) first year registrar positions by 2016, 847 (19.5%) by 2020 and 1265 (26.2%) by 2025. If this happened, there would be literally hundreds of medical graduates who have completed an internship and residency, who would be unable to complete their training in Australia.
With the possibility of future training position shortages, claims that over 50% of current resident medical officers and unaccredited registrars saying that they are not being allocated enough time for structured training and education activities, and medical students such as Skye Kinder and Ben Veness calling for more training places, it is difficult to argue a case for increasing the number of medical students in Australia, even if a new medical school is in an area in need of more doctors.

